In 2009 the American Society for Bariatric Surgery (ASBS) changed its name to the American Society for Metabolic and Bariatric Surgery (ASMBS) to promote information on the beneficial effects of surgeries for weight loss in treating metabolic diseases, especially Type 2 Diabetes Mellitus (T2DM).
Today, the term Metabolic Surgery is used to describe surgical procedures to treat metabolic diseases, especially, type 2 diabetes.
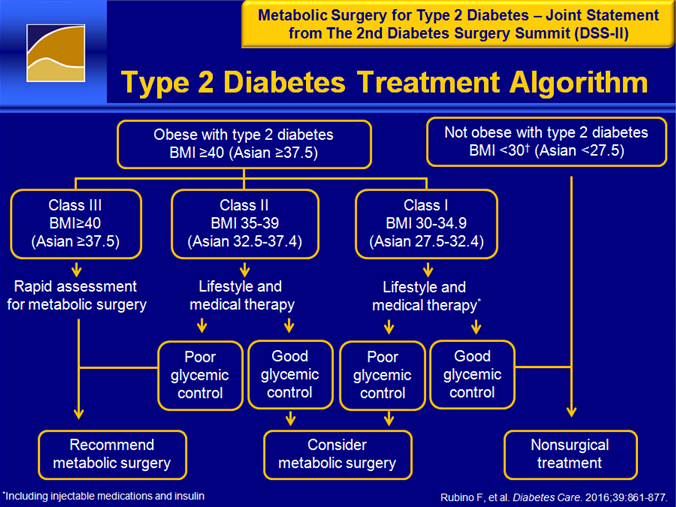
Metabolic Surgery in the Treatment Algorithm for Type 2 Diabetes.
A Joint Statement by International Diabetes Organizations….
FAQs
DOES METABOLIC SURGERY “CURE” DIABETES?
Till date, diabetes is poorly understood and medical treatment cannot claim a “Cure”. The aim is to put it in remission, defined as normal blood sugar levels and no need for diabetes medication. This means bringing glucose to normal levels and arresting the progression of the diabetic complications, thus giving the body a chance to repair the damage.
In 2004, study in Journal of the American Medical Association (JAMA) of more than 22,000 people who underwent bariatric surgery showed the following:
- Diabetes was completely resolved or improved in 86% of patients.
- High blood lipids improved in 70% or more of patients.
- High blood pressure was resolved or improved in 78% of patients.
METABOLIC SURGERY IN TYPE 2 DIABETIC PATIENTS WHO ARE NOT MORBIDLY OBESE?
Actually, 2/3 of the world’s type 2 diabetics are not morbidly obese. They are however, overweight with BMI range 27-35Kg/m2. According to IDF guidelines for Asians, most of metabolic surgeons will accept patients with type 2 diabetes and BMI of 27.5Kg/m2 or greater for metabolic surgery.
It is possible that metabolic surgery may benefit even person with diabetes who are not overweight or obese.
International Diabetes Federation – 2011 Position Statement for Bariatric Surgery
- Obesity and type 2 diabetes are serious chronic diseases associated with complex metabolic dysfunctions that increase the risk for morbidity and mortality.
- The dramatic rise in the prevalence of obesity and diabetes has become a major global public health issue and demands urgent attention from governments, health care systems and the medical community.
- Bariatric surgery is an appropriate treatment for people with type 2 diabetes and obesity not achieving recommended treatment targets with medical therapies, especially when there are other major co-morbidities.
- Surgery should be an accepted option in people who have type 2 diabetes and a BMI of 35 or more.
- Surgery should be considered as an alternative treatment option in patients with a BMI between 30 and 35 when diabetes cannot be adequately controlled by optimal medical regimen, especially in the presence of other major cardiovascular disease risk factors.
- In Asian, and some other ethnicities of increased risk, BMI action points may be reduced by 2.5 kg/m2.
- The morbidity and mortality associated with bariatric surgery is generally low, and similar to that of well-accepted procedures such as elective gall bladder or gall stone surgery. Bariatric surgery for type 2 diabetes must be performed within accepted international and national guidelines. This requires appropriate assessment for the procedure and comprehensive and ongoing multidisciplinary care, patient education, follow-up and clinical audit, as well as safe and effective surgical procedures.
WHO ARE ELIGIBLE TO UNDERGO METABOLIC SURGERY?
- Patients aged between 30 to 65 years, with diabetes> 3 years, not losing weight in the past 1 year, on stable insulin or oral hypoglycemic agents requirement in the past 3 months, post prandial serum C – peptide levels > 0.9 ng/ml
- BMI ≥ 27.5 kg/mt2 with uncontrolled type 2 diabetes
TYPES OF METABOLIC SURGERIES
- Loop Duodenojejunal Bypass With Sleeve Gastrectomy
- Laparoscopic Roux-En-Y Gastric Bypass (Metabolic)
- Sleeve Gastrectomy With Proximal Jejunal Bypass
- Ileal Interposition With Sleeve Gastrectomy
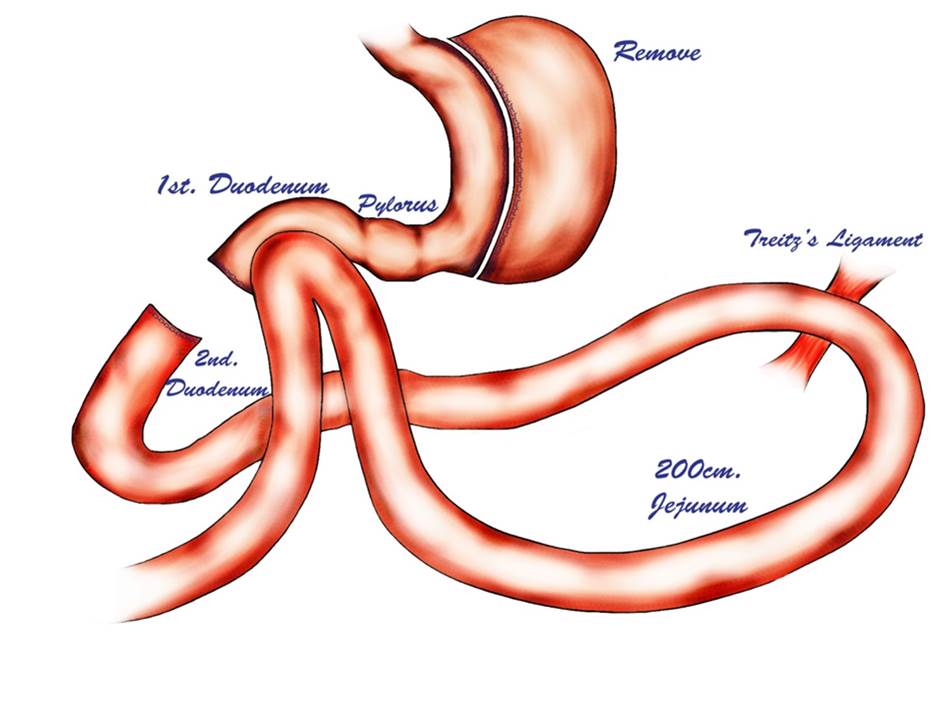
Loop duodenojejunal bypass with sleeve Gastrectomy (LDJB-SG) was started to achieve Type 2 diabetes remission and to avoid the drawbacks of RYGB. It is safe, feasible, and shows good efficacy in terms of glycemic control or long term remission of type 2 diabetes, due to several hormonal changes such as reduced ghrelin,increased GLPI and peptide YY. Adding intestinal diversion to sleeve increases its efficacy and reduces problem related with gastric bypass.Bilio-pancreatic diversion with duodenal switch is the most effective metabolic surgery since hormonal changes are maximum.
FAQs
How metabolic surgery causes diabetes remission?
LDJB-SG causes neuro-hormonal and absorption changes, which result in long-term control of
diabetes.
Sleeve gastrectomy causes caloric restriction and suppresses the anti-insulin effect of ghrelin
hormone. Removal of body of stomach alters gastric empting, causing early satiety and also
changes energy balance. Reduced appetite, improved satiety, increased energy expenditure
and resetting the “set point for food storage” to a lower level result in long-term control of
diabetes.
Exclusion of the proximal intestine suppresses the anti-incretin hormones, which are stimulated
by presence of food in the duodenum. Swifter delivery of food to the distal intestine stimulates
the secretion of incretins like GLP-1 and peptide YY. GLP-1 increases the insulin secretion by
enhancing the function of insulin producing beta cells in pancreas.
For metabolic surgery patients are properly screened and surgery is recommend only for
patients with uncontrolled Type 2 diabetes on Insulin therapy with C-peptide >1, HbA1c > 7 and
BMI > 27.5. Though, metabolic surgery is cost effective, it has minimal complications and
mortality. The future of complete remission of diabetes lies in metabolic surgery.
Can the surgery cause hypoglycemia (low blood sugar)?
After the operation, as in every normal human, insulin will increase after eating. The possibility for hypoglycemia occurrence will decrease continuously and be eliminated during the period after the operation.
Is this pancreas surgery?
No. The performed processes are basically a displacement process performed in the small intestine. In addition to this, in situations where it is deemed necessary deemed (depending on the disease level, the hormone levels in the blood and the activity of these hormones), required surgical operations regarding the stomach volume, stomach form and the fatty tissues wrapping the organs in the abdomen are performed.
Will I need to take supplements after metabolic surgery?
To avoid long term micro nutrient deficiency, it is advisable to take regular supplements.
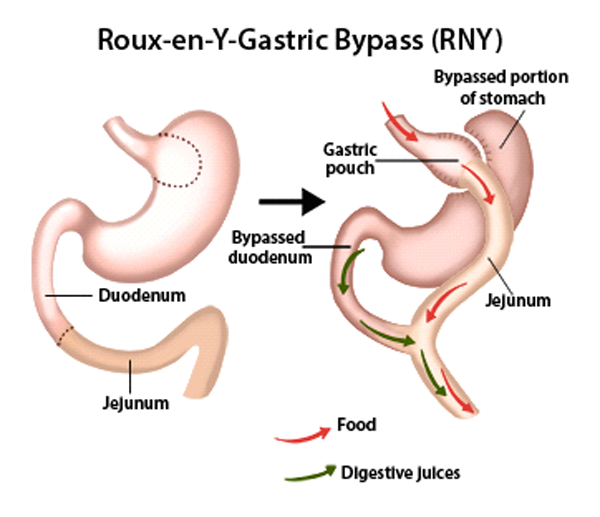
Laparoscopic roux-en-Y Gastric Bypass (Metabolic) is a reversible weight loss procedure that reduces the size of your stomach to a small 30cc pouch and making food bypass the beginning of the small intestine. This reduces your appetite and makes you feel satiated with smaller portions. LRYGB can help you lose up to 60 – 80% of your excess weight in a period of approximately 2 years.
For more information
Less
FAQs
How metabolic surgery causes diabetes remission?
LDJB-SG causes neuro-hormonal and absorption changes, which result in long-term control of
diabetes.
Sleeve gastrectomy causes caloric restriction and suppresses the anti-insulin effect of ghrelin
hormone. Removal of body of stomach alters gastric empting, causing early satiety and also
changes energy balance. Reduced appetite, improved satiety, increased energy expenditure
and resetting the “set point for food storage” to a lower level result in long-term control of
diabetes.
Exclusion of the proximal intestine suppresses the anti-incretin hormones, which are stimulated
by presence of food in the duodenum. Swifter delivery of food to the distal intestine stimulates
the secretion of incretins like GLP-1 and peptide YY. GLP-1 increases the insulin secretion by
enhancing the function of insulin producing beta cells in pancreas.
For metabolic surgery patients are properly screened and surgery is recommend only for
patients with uncontrolled Type 2 diabetes on Insulin therapy with C-peptide >1, HbA1c > 7 and
BMI > 27.5. Though, metabolic surgery is cost effective, it has minimal complications and
mortality. The future of complete remission of diabetes lies in metabolic surgery.
Can the surgery cause hypoglycemia (low blood sugar)?
After the operation, as in every normal human, insulin will increase after eating. The possibility for hypoglycemia occurrence will decrease continuously and be eliminated during the period after the operation.
Is this pancreas surgery?
No. The performed processes are basically a displacement process performed in the small intestine. In addition to this, in situations where it is deemed necessary deemed (depending on the disease level, the hormone levels in the blood and the activity of these hormones), required surgical operations regarding the stomach volume, stomach form and the fatty tissues wrapping the organs in the abdomen are performed.
Will I need to take supplements after metabolic surgery?
To avoid long term micro nutrient deficiency, it is advisable to take regular supplements.
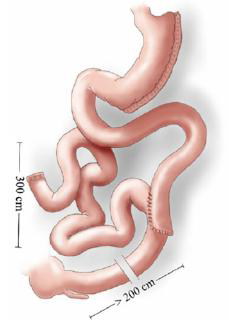
Sleeve Gastrectomy with proximal jejunal bypass
In this process bypassing a short segment of proximal intestine directly ameliorates type 2 diabetes, independently of effects on food intake, body weight, malabsorption, or nutrient delivery to the hindgut. These findings suggest that a proximal intestinal bypass could be considered for diabetes treatment and that potentially undiscovered factors from the proximal bowel might contribute to the pathophysiology of type 2 diabetes.
FAQs
How metabolic surgery causes diabetes remission?
LDJB-SG causes neuro-hormonal and absorption changes, which result in long-term control of
diabetes.
Sleeve gastrectomy causes caloric restriction and suppresses the anti-insulin effect of ghrelin
hormone. Removal of body of stomach alters gastric empting, causing early satiety and also
changes energy balance. Reduced appetite, improved satiety, increased energy expenditure
and resetting the “set point for food storage” to a lower level result in long-term control of
diabetes.
Exclusion of the proximal intestine suppresses the anti-incretin hormones, which are stimulated
by presence of food in the duodenum. Swifter delivery of food to the distal intestine stimulates
the secretion of incretins like GLP-1 and peptide YY. GLP-1 increases the insulin secretion by
enhancing the function of insulin producing beta cells in pancreas.
For metabolic surgery patients are properly screened and surgery is recommend only for
patients with uncontrolled Type 2 diabetes on Insulin therapy with C-peptide >1, HbA1c > 7 and
BMI > 27.5. Though, metabolic surgery is cost effective, it has minimal complications and
mortality. The future of complete remission of diabetes lies in metabolic surgery.
Can the surgery cause hypoglycemia (low blood sugar)?
After the operation, as in every normal human, insulin will increase after eating. The possibility for hypoglycemia occurrence will decrease continuously and be eliminated during the period after the operation.
Is this pancreas surgery?
No. The performed processes are basically a displacement process performed in the small intestine. In addition to this, in situations where it is deemed necessary deemed (depending on the disease level, the hormone levels in the blood and the activity of these hormones), required surgical operations regarding the stomach volume, stomach form and the fatty tissues wrapping the organs in the abdomen are performed.
Will I need to take supplements after metabolic surgery?
To avoid long term micro nutrient deficiency, it is advisable to take regular supplements.
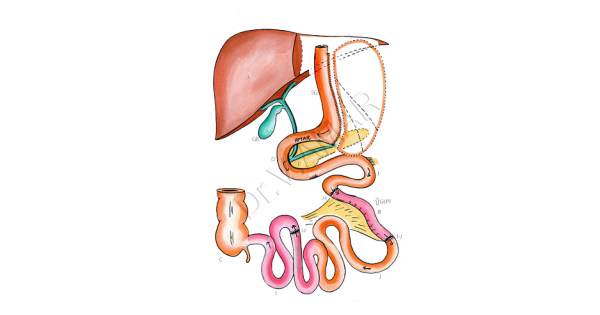
Ileal Interposition is a laparoscopic operation for control of Type-2 Diabetes in which a long segment of last part of small bowel (Ileum) is cut & joined very close to the stomach. This results in several hormonal changes such as reduced Ghrelin, increased GLP1 and Peptide YY. These hormonal changes results in resolution or long term remission of type 2 diabetes (T2D). Undigested food now first enters Ileum to stimulate increased secretion of incretin (gut) hormone called GLP-1, which stimulates beta cells in pancreas to secrete increase amounts of insulin, provided enough Beta Cell mass is still present in pancreas. Persistent increased GLP-1 secretion increases Beta Cell mass in the long term.
Advantage:
- Operation for control of Type-2 diabetes even with normal BMI (Non obese patients)
Disadvantage:
- There is slight risk of vitamin and mineral deficiencies.
FAQs
How metabolic surgery causes diabetes remission?
LDJB-SG causes neuro-hormonal and absorption changes, which result in long-term control of
diabetes.
Sleeve gastrectomy causes caloric restriction and suppresses the anti-insulin effect of ghrelin
hormone. Removal of body of stomach alters gastric empting, causing early satiety and also
changes energy balance. Reduced appetite, improved satiety, increased energy expenditure
and resetting the “set point for food storage” to a lower level result in long-term control of
diabetes.
Exclusion of the proximal intestine suppresses the anti-incretin hormones, which are stimulated
by presence of food in the duodenum. Swifter delivery of food to the distal intestine stimulates
the secretion of incretins like GLP-1 and peptide YY. GLP-1 increases the insulin secretion by
enhancing the function of insulin producing beta cells in pancreas.
For metabolic surgery patients are properly screened and surgery is recommend only for
patients with uncontrolled Type 2 diabetes on Insulin therapy with C-peptide >1, HbA1c > 7 and
BMI > 27.5. Though, metabolic surgery is cost effective, it has minimal complications and
mortality. The future of complete remission of diabetes lies in metabolic surgery.
Can the surgery cause hypoglycemia (low blood sugar)?
After the operation, as in every normal human, insulin will increase after eating. The possibility for hypoglycemia occurrence will decrease continuously and be eliminated during the period after the operation.
Is this pancreas surgery?
No. The performed processes are basically a displacement process performed in the small intestine. In addition to this, in situations where it is deemed necessary deemed (depending on the disease level, the hormone levels in the blood and the activity of these hormones), required surgical operations regarding the stomach volume, stomach form and the fatty tissues wrapping the organs in the abdomen are performed.
Will I need to take supplements after metabolic surgery?
To avoid long term micro nutrient deficiency, it is advisable to take regular supplements.